Cardiac arrest survival depends on one factor above all others — the quality and continuity of CPR. Every second of interrupted chest compressions reduces blood flow to the brain and heart. Two-rescuer CPR exists precisely to solve this problem.
Introduction
When cardiac arrest occurs, the heart stops pumping oxygenated blood to vital organs. Brain damage begins within four to six minutes of circulatory collapse. Effective CPR maintains enough blood flow to preserve brain function until advanced care restores a normal rhythm.
Single-rescuer CPR is physically demanding and inherently limited. One person cannot sustain high-quality compressions indefinitely while also managing the airway. Fatigue sets in quickly, and compression quality degrades within two minutes, even in well-trained individuals.
Two-rescuer CPR addresses these limitations directly. By dividing responsibilities between two trained providers, the team maintains higher compression quality, reduces fatigue-related errors, and integrates AED use without sacrificing perfusion pressure. The goal is simple — no pauses, no compromises, no gaps in circulation.
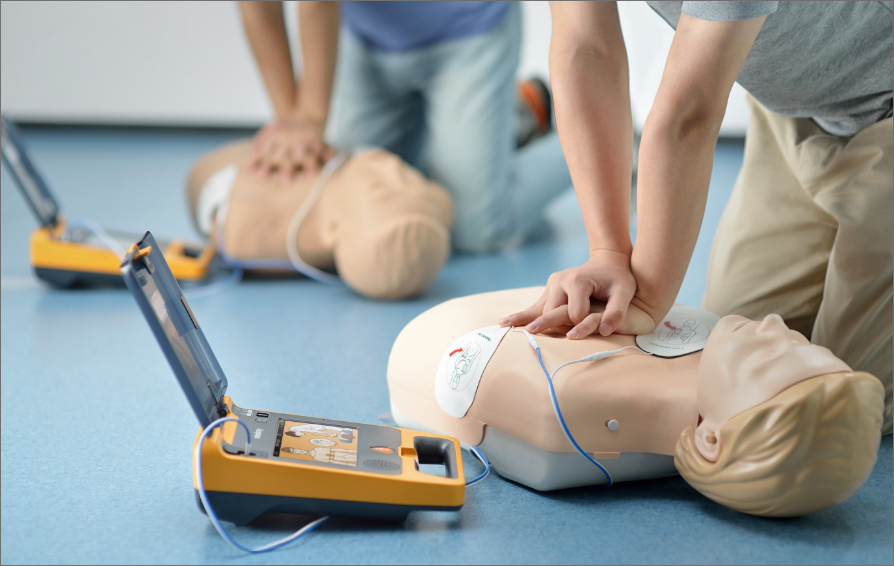
Why Two-Rescuer CPR is More Effective
Research consistently demonstrates that two-rescuer CPR produces better outcomes than single-rescuer efforts. A study published in Resuscitation found that compression depth and rate decline significantly after just 90 seconds of continuous single-rescuer CPR. Two rescuers eliminate this degradation through structured role rotation.
The physiological case for uninterrupted compressions is compelling. Coronary perfusion pressure — the driving force that keeps blood moving through the heart — takes approximately 30 seconds to build after compressions begin. Every pause resets this pressure to zero. Minimizing interruptions preserves the perfusion pressure that single-rescuer CPR repeatedly destroys.
Call Us Now
Get the Best CPR Class in Indianapolis Today!
Two-rescuer CPR offers distinct advantages over solo response:
- Sustained compression quality — Rotation every two minutes prevents fatigue-related depth and rate decline
- Simultaneous airway management — One rescuer handles ventilations while the other maintains compressions
- Faster AED integration — Pad application and rhythm analysis are performed without stopping compressions
- Improved team communication — Role clarity reduces hesitation and errors during high-stress response
- Better patient outcomes — Consistent perfusion pressure is directly associated with higher rates of return of spontaneous circulation (ROSC)
The American Heart Association emphasizes that high-quality CPR is defined by rate, depth, full chest recoil, minimal interruptions, and appropriate ventilation. Two rescuers are simply better positioned to deliver all five elements simultaneously.
How to Perform 2-Person CPR: Step-by-Step
Effective two-rescuer CPR begins with clear role assignment before compressions start. Confusion about responsibilities wastes time and creates dangerous gaps. Each rescuer must know their position and task from the first moment of response.
Step 1 — Scene Safety and Assessment
Confirm the scene is safe before approaching. Assess the patient for responsiveness by tapping the shoulders firmly and calling out loudly. If there is no response and no normal breathing, cardiac arrest is assumed.
Step 2 — Activate Emergency Services
One rescuer calls 911 or directs a bystander to call immediately. The other rescuer begins chest compressions without delay. Do not wait for the phone call to finish before starting CPR.
Step 3 — Assign Roles
- Rescuer 1 — Compressor: Positioned at the patient’s side, responsible for delivering chest compressions
- Rescuer 2 — Airway Manager: Positioned at the patient’s head, responsible for maintaining the airway and delivering ventilations
Step 4 — Begin Chest Compressions
The compressor places the heel of one hand on the center of the chest at the lower half of the sternum. The second hand is placed on top with fingers interlaced. Arms are kept straight with shoulders directly over the hands.
Compressions are delivered at:
- Rate — 100 to 120 compressions per minute
- Depth — At least 2 inches for adults
- Recoil — Full chest recoil allowed between each compression
- Interruptions — Kept to an absolute minimum; no pause longer than 10 seconds
Step 5 — Airway and Ventilation
The airway manager opens the airway using a head-tilt chin-lift. A bag-valve mask (BVM) is used when available. Two breaths are delivered after every 30 compressions in single-rescuer ratio; two trained rescuers switch to 15:2 for adult patients.
Each breath is delivered over one second. The chest should visibly rise with each ventilation. Avoid excessive force, which causes gastric inflation and reduces lung compliance.
Step 6 — Rotate Compressors
Rotation occurs every two minutes or at the end of each five-cycle block. The switch is made as quickly as possible — ideally in under five seconds. The incoming compressor positions themselves before the rotation is called so the transition is seamless.
Two-Rescuer CPR with AED: The Correct Sequence
AED integration is where two-rescuer coordination becomes most critical. Incorrect sequencing causes unnecessary pauses that reduce the chance of successful defibrillation. The correct sequence keeps compressions running until the last possible moment before a shock.
The correct AED integration sequence:
- Retrieve and power on the AED — The airway manager activates the AED while the compressor continues uninterrupted compressions
- Apply pads without stopping compressions — Pads are placed while compressions continue; one pad below the right collarbone, one on the left side below the armpit
- Analyze rhythm on cue — When the AED prompts analysis, the compressor pauses only at that moment; the pause must be under 10 seconds
- Clear and deliver shock — Confirm no one is in contact with the patient, deliver the shock, and immediately resume compressions
- Resume compressions within five seconds of shock — Do not wait for rhythm analysis or signs of ROSC before restarting compressions
The AHA specifies that the preshock pause — the time between the last compression and the delivery of shock — should be kept to under five seconds. Research shows that each additional second of preshock pause reduces the likelihood of successful defibrillation. Speed and coordination at this moment directly influence survival.
Post-shock compressions are non-negotiable. The heart requires support immediately after defibrillation while it attempts to reestablish an organized rhythm. Waiting to see whether the shock worked before resuming compressions wastes the perfusion window created by compressions.
Compression-to-Ventilation Ratios for Two Rescuers
Ratio selection is one of the most important protocol decisions in two-rescuer CPR. The correct ratio depends on the patient’s age and whether an advanced airway is in place. Using the wrong ratio reduces either perfusion or oxygenation effectiveness.
Standard ratios for two trained rescuers:
- Adult patients (no advanced airway) — 30 compressions to 2 ventilations
- Pediatric patients (no advanced airway) — 15 compressions to 2 ventilations; this is the key distinction for two trained rescuers
- All patients (with advanced airway in place) — Continuous compressions at 100 to 120 per minute with one breath delivered every 6 seconds asynchronously
The pediatric 15:2 ratio reflects the respiratory origin of most pediatric cardiac arrests. More frequent ventilations address the underlying hypoxia that triggered the arrest. This ratio applies to children from age one through puberty and requires two trained rescuers to execute correctly.
Once an advanced airway such as an endotracheal tube or supraglottic airway is in place, the ratio-based approach is abandoned entirely. Compressions run continuously without pause for ventilations. The airway manager delivers one breath every six seconds independently of the compression cycle.
Minimizing Pauses: Advanced Coordination Techniques
Pause minimization is the defining characteristic of high-performance two-rescuer CPR. Every protocol decision and coordination habit should be evaluated through one lens — does this reduce interruptions to compressions? Advanced teams treat pause prevention as an active, practiced discipline.
Techniques used by high-performance resuscitation teams include:
- Pre-positioning for rotation — The incoming compressor kneels into position and places hands before calling the switch, reducing transition time to under three seconds
- Verbal countdown before rotation — The compressor calls out the last five compressions of each cycle, so the team prepares simultaneously
- Hands-on defibrillation preparation — AED pads are connected, and the device is powered during compressions, not after
- Continuous compressions during BVM ventilation — Advanced teams trained in asynchronous CPR deliver ventilations between compressions without formal pauses
- Closed-loop communication — Every instruction from the team leader is verbally confirmed by the receiving rescuer to eliminate misunderstanding
- Dedicated rhythm checker — One rescuer is assigned to interpret the AED output, so the compressor never needs to divert attention
Real-time feedback devices are a powerful tool for maintaining compression quality. Devices that measure rate, depth, and recoil provide immediate data to both the compressor and the team leader. Studies published in the Journal of the American Heart Association found that feedback devices significantly improve guideline-compliant compression delivery.
Special Considerations and Scenarios
Two-rescuer CPR must adapt to a range of patient presentations and environmental conditions. Protocol fundamentals remain constant, but practical execution requires flexibility. Prepared rescuers anticipate these variables before they arise.
Pregnant patients — The uterus compresses the inferior vena cava in the supine position, reducing venous return. Manual left uterine displacement is applied continuously while compressions are performed. Standard hand placement and depth apply; do not modify compression technique for pregnancy.
Pediatric patients — The two-finger technique is replaced by the two-thumb encircling technique when two rescuers are present. Both thumbs are placed on the lower third of the sternum, and fingers wrap around the torso. This method produces superior compression depth and recoil in infants compared to the two-finger technique.
Obese patients — Increased chest wall resistance may require additional compression force to achieve adequate depth. Hand placement remains the same. Rescuers should confirm visible chest recoil rather than relying solely on the force applied.
Confined spaces — Limited access may prevent standard side-by-side positioning. An over-the-head compressor position can be used when side access is not available. Airway management may require adaptation based on available angles.
Suspected spinal injury — Head-tilt chin-lift is replaced by jaw thrust to open the airway without neck extension. Compressions are not modified. Spinal precautions are maintained throughout resuscitation where the mechanism of injury suggests spinal trauma.
Training and Skill Maintenance
Two-rescuer CPR cannot be effectively learned through reading alone. The coordination, timing, and physical technique required must be rehearsed on mannequins with a partner. Isolated skill practice does not replicate the communication demands of real team resuscitation.
BLS certification through the AHA includes two-rescuer scenarios for all provider-level courses. Skills stations are evaluated by instructors using standardized performance criteria. Certification is valid for two years, but skill quality degrades significantly without regular reinforcement.
Strategies for maintaining two-rescuer proficiency between certifications:
- Scheduled team drills — Monthly or quarterly practice sessions with regular co-responders reinforce team coordination
- Mannequin skills labs — Many hospitals and training centers offer open practice time outside of formal courses
- Video-assisted debriefing — Reviewing recorded resuscitation attempts identifies coordination gaps invisible during the event
- Simulation-based training — High-fidelity simulation scenarios expose teams to low-frequency, high-acuity presentations in a controlled environment
- Individual compression practice — Regular solo compression sessions maintain physical conditioning and technique accuracy
The AHA recommends that healthcare teams engage in resuscitation debriefing after every cardiac arrest event. Structured review of timing, role performance, and communication quality accelerates team-level improvement. Learning from real events is one of the most effective training tools available.
FAQs: Two-Person CPR + AED: No Pauses
Q1: Why is eliminating pauses so important during two-person CPR with an AED? Every second of interrupted chest compressions reduces blood flow to the brain and heart. In two-person CPR, roles are divided — one rescuer continues compressions while the other operates the AED — so shocks can be delivered with minimal interruption. This coordinated approach dramatically improves survival outcomes compared to single-rescuer CPR.
Q2: How do the two rescuers coordinate during AED analysis and shock delivery? When the AED begins analyzing the heart rhythm, the compressor pauses only for the brief analysis window. The second rescuer manages the AED, charges it, and ensures everyone is clear before the shock is delivered. Immediately after the shock, compressions resume without delay — keeping that critical no-pause rhythm intact.
Q3: Does two-person CPR with an AED require special training? Yes — proper technique, role switching, and AED coordination all require hands-on practice. A BLS (Basic Life Support) course teaches healthcare providers and trained responders exactly how to execute two-person CPR efficiently. Knowing your role before an emergency makes all the difference.
Conclusion & Call to Action
Two-person CPR combined with an AED is one of the most effective resuscitation techniques available — but only when both rescuers know their roles and minimize interruptions to compressions. The “no pauses” approach is not just a best practice; it’s a life-saving standard that every trained responder should master.
Whether you’re a healthcare professional or a community member looking to be prepared, proper training turns panic into confident action. CPR Indianapolis, an American Heart Association training site, offers stress-free, hands-on courses designed to build real-world skills — not just check a box.
Ready to get trained? Get your CPR certification in Indianapolis — initial certifications and renewals available. Register for a BLS class in Indianapolis — BLS for Healthcare Providers, ACLS, PALS, and CPR & First Aid courses offered year-round.
Don’t wait for an emergency to wish you were prepared. Sign up with CPR Indianapolis today and learn to save a life — no stress, all hands-on.


